Colorectal cancer is one of the most common forms of cancer in Australia and the second biggest cancer killer. Every year, more than 15,000 people are told they have bowel cancer, with more than 2,000 people under the age of 55.
A systematic review and dose-response meta-analysis of 25 prospective cohort studies found that fibre from grains, particularly whole grains, is associated with reduced risk of colorectal cancer, but fibre from fruit and vegetables does not have a significant association. 1 Of course there are numerous health benefits of eating fruit and vegetables, but when it comes to bowel cancer, eating whole grains is one of the best preventative measures.
From an analysis of the eight cohort studies that reported on cereal fibre intake, the review found that for every 10g of cereal fibre, the risk of developing bowel cancer was reduced by 10%. 2 In addition, people who ate 3 serves of whole grain and/or high fibre grain foods per day were 17% less likely to develop bowel cancer than those people who didn’t eat whole grain and/or high fibre grain foods.
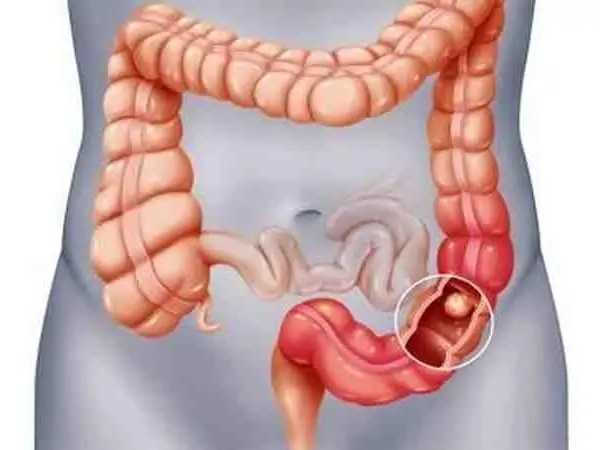
Source: Times of India
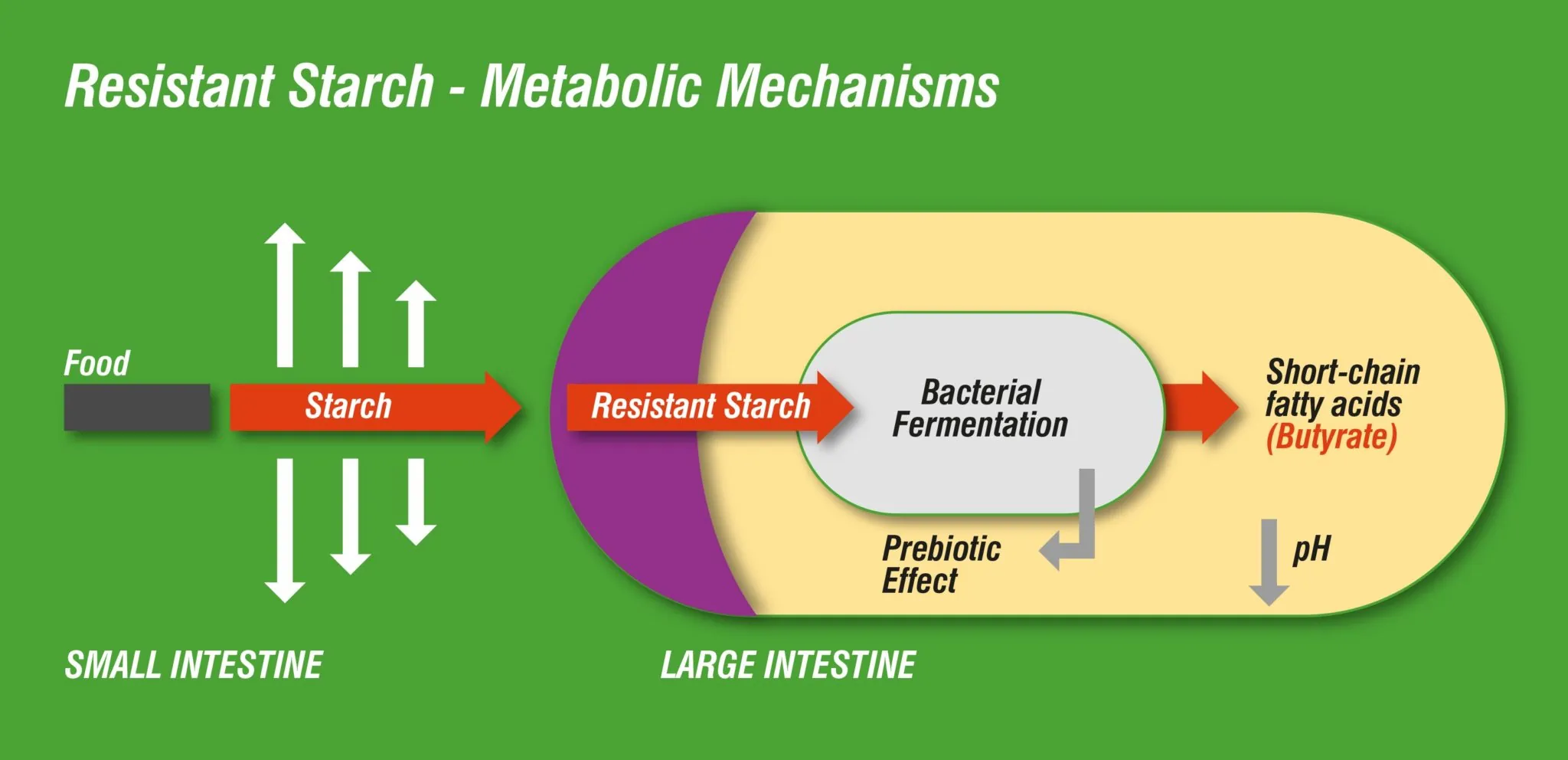
But eating more cereal fibre is not the whole story. Different types of fibre affect the bowel in different ways and each confer unique health benefits. One prebiotic fibre in particular, resistant starch, passes through the intestine undigested, and when it reaches the large bowel, it is fermented by bacteria to produce short chain fatty acids. The main SCFA are acetate, propionate and butyrate. Of these, it is believed that butyrate is of particular benefit for lowering bowel cancer risk as it promotes the death of colorectal cancer cells, and it feeds the beneficial bacteria in the large intestine.3 When these good bacteria are dominant in the gut, they establish an environment that nourishes the cells that line the gut wall and provide important immune signals that establish a healthy immune response.
According to David Topping from the CSIRO, “The paradox in Australia is that while we have one of the highest intakes of fibre in industrialised countries we still have one of the highest rates of bowel cancer. The answer lies not in advice to increase fibre intake generally, but more importantly to eat different types of fibre including foods that contain resistant starch, which promotes the production of butyrate”.
The different composition of dietary fibres in cereals, vegetables and fruit may be the reason why a significant association has been found between bowel cancer risk and cereal fibre consumption, but not vegetable or fruit fibre. Some heterogeneity has also been observed with fibre source and cardiovascular risk reduction. 4 So yet more reason why we need to encourage people to eat a range of food types and ensure adequate intake of all the dietary fibres.
Yours in good health,
Teri Lichtenstein APD
The Healthy Grain Nutrition Ambassador
References:
- Aune, D et al. Dietary fibre, whole grains, and risk of colorectal cancer: systematic review and dose-response meta-analysis of prospective studies. BMJ. 2011;343:d6617
- Bird AR, Vuaran M, Crittenden R, Hayakawa T, Playn MJ, Brown IL and Topping DL. Comparative effects of a high-amylose starch and a fructooligosaccharide on fecal bifidobacteria numbers and short-chain fatty acids in pigs fed Bifidobacterium animalis. Digestive Diseases and Sciences. 2009; 54: 947-954.
- Bird T et al. Resistant starch, large bowel fermentation and broader perspective of prebiotics and probiotics. Benef Microbes. 2010; 1(4):423-31
- Dietary fibre intake and risk of cardiovascular disease: systematic review and meta-analysis.
Intended as general advice only. Consult your health care professional to discuss any specific concerns.







5 Comments